One of the things that most fuels self-deception is imagining that we should be living, or maybe even still live, in what we imagine was a better past. Of course, the past was not always better – in fact, it was overall, for most people, worse – but our minds repress the bad and remember the good from when we were children, as I have discussed in my other blog, “Life, the Universe, and a Few Things” (Brooklyn Nostalgia, August 21, 2011). Sometimes there is a conscious effort, a movement if you will, to block out the really bad things that have happened in the past not only from our individual memory but from our history books and schools. Clearly, this is happening now with regard to the primary founding evils in US history, extermination of the indigenous inhabitants (Native Americans, Indians) and slavery. That these were real is incontrovertible. That they were horrific, inexcusable, and must be remembered both to honor the victims and prevent recurrence should be obvious. But the effort to suppress teaching of this history, parallel to suppressing teaching about the Holocaust (which is not suppressed in Germany) is ongoing, vicious and wrong. To add insult to injury, advocates are adopting the language of microaggression, justifying their racist efforts to whitewash history with ostensible concern for “making white children feel bad about themselves”.
This is, in addition to every other evil and reprehensible aspect of it, also a way to divert those children – and their parents – from knowing and worrying about the things that they should be worried about, such as climate change and nuclear war. And the incredible inequities in American society (not to mention the world!) that have actually led to terrible social and individual outcomes. For example, the drop in life expectancy in the US. Yes, drop. People living shorter lives than they used to. Due in part to the COVID pandemic, but due in the US more to the vast inequities in wealth, social support, access to health care, jobs, use of harmful substances (such as alcohol, opioids, and tobacco) and every other determinant of health. What this has to do with self-deception and living in the past is the false idea that things are always, automatically, better in this country, the USA, a belief that persists in the face of evidence.
Of course, some things were, in fact, better in this country for earlier generations, some of whose members are still alive and sentient. America may not have always welcomed its immigrants, even those from Europe, and viciously and continuously repressed and oppressed members of many minority groups (particularly Natives and the descendants of Black slaves), but in the first half of the 20th century, major parts of life were often better here for poor people than in many other countries. This was even more so after World War II, when the economies of most of the rest of the developed world were destroyed but the US' was intact, with no wars fought on its soil. This resulted in great success for US manufacturers (no competition!) and other benefits. One was life expectancy, due in large part to better nutrition. In the second half of the 20th century it was widely observed that children of immigrants were bigger than their parents, because from infancy they were better nourished. Then, even later, at the end of that century and into the 21st, some of the major causes of premature death saw a decline, mainly tobacco use.
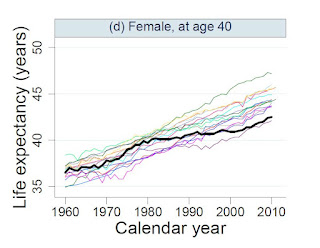
But the premature death rate in the US is going up, life expectancy is going down. An important paper, published in 2014 in the Annual Review of Public Health by Mauricio Avenando and Ichiro Kawachi, ‘Why do Americans have shorter life expectancy and worse health than people in other high-income countries?’, provides extensive documentation and discussion, including a supplement with several tables comparing life expectancy among different countries (a representative one, Female Life Expectancy at 40, is reproduced here).
While it has long, forever, been true that the life expectancy of underserved minority populations was less than for white people, the decrease in life expectancy for the “majority” group was shockingly revealed by data provided in 2015 by economists Anne Case and Angus Deaton, “Rising morbidity and mortality in midlife among white non-Hispanic Americans in the 21st century”, and has been demonstrated for larger and larger portions of the US population. As I noted in this blog (Rising white midlife mortality: what are the real causes and solutions?, November 14, 2015) this was a shock for those who held to the belief that it was only true for minorities (and in perverted way, found this reassuring). Indeed, while the life expectancy for Black Americans was and is still shorter than for whites, it was slowly rising while for many whites (of course, especially lower-income whites) it was dropping. Case and Deaton, noting the large increase in mid-life death (kind of an oxymoron, but meaning “middle age”) attributed this to “deaths of despair”, specifically due to opioids and suicide. On November 29, 2019 I wrote about an article by Steven Woolf and Heidi Schoonmaker, “Life Expectancy and Mortality Rates in the United States, 1959-2017” (Decreasing life expectancy in the US: A result of policies fostering increasing inequity), and I noted that, amazingly, women in lower income groups born in 1950 had shorter life expectancies than their mothers born in 1920!
Woolf and his colleagues RK Masters and LY Aron have recently come out with a new publication looking at life expectancy in the US and other OECD countries for 2019-2021. (Note: at the time of publication, the paper, in medRxiv, had not been peer-reviewed). They found that the pandemic shortened the life expectancy in almost all countries, but
US life expectancy decreased from 78.86 years in 2019 to 76.99 years in 2020 and 76.60 years in 2021, a net loss of 2.26 years. In contrast, peer countries averaged a smaller decrease in life expectancy between 2019 and 2020 (0.57 years) and a 0.28-year increase between 2020 and 2021, widening the gap in life expectancy between the United States and peer countries to more than five years.
In addition, ‘The decrease in US life expectancy was highly racialized: whereas the largest decreases in 2020 occurred among Hispanic and non-Hispanic Black populations, in 2021 only the non-Hispanic White population experienced a decrease in life expectancy.’ So while in 2020 the most vulnerable populations took the greatest additional hit from COVID, by 2021 they were slowly recovering, while white populations continued to lose life expectancy.
So why? This may be cognitive dissonance for the self-deluding, or racist, or narrow-minded, or those who think “America is always better”, but it is true. And the reasons for it are the inequities of American life, much of which is detailed in the Avenando and Kawachi paper, as well as Masters, Aron, and Woolf. We do not have universal health insurance, and we do not have universal access to health care. Even many “insured” Americans have very poor insurance, many Americans do not have geographic or physical access to health care services, and thus many people forego health care altogether or until it is too late. Our infant mortality rate is far higher than that of comparable countries. We still have large numbers of people who are “food insecure”, which often means chronically hungry and undernourished, not to mention those who are “housing insecure”, often homeless. And we have phenomenal income inequities which have grown tremendously since the 1980s Reagan assault on the social safety net. A paper by economists Emanuel Saez and Gabriel Zucman, widely covered, shows examples of this: since 1982 the wealth of the 0.00001% (18 families!) has increased from 0.1% to 1.2% of all US wealth.
Just from 2009-2022 the wealthiest American has gone from $40B to $265B, while average income has decreased from $54,283 to $53,490, and the minimum wage ($7.25/hr) has stayed the same! So the US remains an outlier, with great social and economic inequity, poorer health, and shorter (and decreasing) life expectancy. You can believe what you want in terms of political and social theory, but you have to be willing to accept the consequences.
I find these consequences, completely unnecessary, intolerable.